Ankylosing spondylitis

Ankylosing spondylitis
Ankylosing Spondylitis: Unveiling Symptoms, Causes, and Types
Ankylosing spondylitis (AS) is a chronic inflammatory arthritis that primarily affects the spine. This condition causes inflammation of the spinal joints, leading to pain, stiffness, and, over time, the fusion of vertebrae. Ankylosing spondylitis belongs to a group of inflammatory arthritis conditions known as spondyloarthritis.
Symptoms:
- Back Pain: Persistent and often severe lower back pain, usually worse in the morning or after periods of inactivity.
- Stiffness: Stiffness and reduced mobility in the spine, especially in the morning or after prolonged periods of rest.
- Enthesitis: Inflammation at the sites where ligaments and tendons attach to bones, leading to pain and swelling, commonly affecting the heels and chest wall.
- Fatigue: General fatigue and a feeling of being unwell, which may result from the ongoing inflammation.
- Reduced Chest Expansion: Inflammation of the spine can lead to decreased flexibility of the chest wall, reducing the ability to expand the chest fully.
Causes:
- Genetic Predisposition: Ankylosing spondylitis has a strong genetic component, with a specific gene called HLA-B27 associated with an increased risk. However, not everyone with HLA-B27 develops the condition, and some individuals without this gene can still be affected.
- Immune System Dysfunction: Ankylosing spondylitis is characterized by an overactive immune system that mistakenly attacks the joints and entheses, leading to inflammation and tissue damage.
- Environmental Factors: While genetics play a significant role, environmental factors, such as infections, may trigger the onset of ankylosing spondylitis in genetically predisposed individuals.
Types of Ankylosing Spondylitis:
- Classic Ankylosing Spondylitis: This is the most common type, characterized by inflammation primarily affecting the spine, especially the sacroiliac joints. Over time, fusion of the vertebrae may occur, leading to reduced flexibility.
- Peripheral Spondyloarthritis: In addition to spinal involvement, this type includes inflammation of peripheral joints (joints other than the spine), such as knees, ankles, or shoulders.
- Non-Radiographic Axial Spondyloarthritis: In some cases, individuals may experience symptoms consistent with ankylosing spondylitis, but radiographic evidence of spinal damage is not initially present. Over time, these individuals may progress to classic ankylosing spondylitis.
Prognosis:
– Ankylosing spondylitis is a chronic condition, and the prognosis varies among individuals.
– Early diagnosis and appropriate management can significantly improve symptoms and quality of life.
– Complications such as spinal fusion can limit mobility, but proactive treatment can help delay or mitigate these effects.
In conclusion, ankylosing spondylitis is a complex inflammatory arthritis with a range of symptoms and potential outcomes. Understanding its causes, recognizing symptoms, and implementing a comprehensive treatment approach are vital for effectively managing this condition.
Guillain Barre Syndrome
Guillain Barre Syndrome
Guillain-Barré syndrome (GBS) is a rare neurological disorder where the body’s immune system mistakenly attacks the peripheral nerves. This can lead to weakness, numbness, and in severe cases, paralysis. Here’s an overview of Guillain-Barré syndrome, including its symptoms, causes, and types:
Symptoms of Guillain-Barré Syndrome:
- Muscle Weakness:
– Progressive weakness, usually starting in the legs and often spreading to the arms. Weakness can range from mild to severe.
- Tingling and Numbness:
– Sensations of tingling or numbness in the extremities are common early signs of Guillain-Barré syndrome.
- Loss of Reflexes:
– A decrease or absence of reflexes, especially the deep tendon reflexes, is a characteristic feature.
- Difficulty with Motor Skills:
– Patients may experience difficulty with motor skills, including walking, grasping objects, or performing other coordinated movements.
- Pain and Aches:
– Some individuals with GBS may experience pain and aching sensations, often in the affected limbs.
- Breathing Difficulties:
– In severe cases, GBS can lead to respiratory muscle weakness, causing breathing difficulties and the need for ventilatory support.
- Difficulty Swallowing and Speaking:
– Weakness in the muscles responsible for swallowing and speaking can occur, leading to dysphagia and dysarthria.
- Autonomic Dysfunction:
– GBS can affect the autonomic nervous system, leading to issues like fluctuations in blood pressure, heart rate abnormalities, and problems with bowel and bladder function.
Causes of Guillain-Barré Syndrome:
- Infections:
– The most common trigger for GBS is infection, often a respiratory or gastrointestinal infection caused by bacteria or viruses. Notable associations include Campylobacter jejuni, Cytomegalovirus (CMV), and the Epstein-Barr virus.
- Immune Response:
– GBS is thought to result from the body’s immune system mistakenly attacking the myelin sheath or peripheral nerves, disrupting nerve function.
- Vaccinations:
– While extremely rare, certain vaccinations, particularly the influenza vaccine and some vaccines against viruses like the Zika virus, have been associated with GBS.
- Surgery:
– Surgical procedures can, in rare cases, trigger GBS. However, the exact mechanisms are not fully understood.
- Trauma or Injury:
– Physical trauma or injury, though uncommon, has been linked to the development of Guillain-Barré syndrome.
Types of Guillain-Barré Syndrome:
- Acute Inflammatory Demyelinating Polyneuropathy (AIDP):
– This is the most common form of GBS, characterized by inflammation and damage to the myelin sheath of peripheral nerves.
- Miller Fisher Syndrome (MFS):
– MFS is a variant of GBS that typically involves ophthalmoplegia (paralysis of eye muscles), ataxia, and areflexia. It is associated with antibodies against a specific nerve cell component.
- Acute Motor Axonal Neuropathy (AMAN):
– AMAN is characterized by motor nerve damage without significant demyelination. It often presents with rapid-onset motor weakness and is more prevalent in certain regions.
- Acute Motor Sensory Axonal Neuropathy (AMSAN):
– Similar to AMAN but involves both motor and sensory nerve damage. It is a more severe and less common subtype.
- Bifacial Weakness with Paresthesias (BFP):
– BFP is characterized by weakness in the muscles innervated by the facial nerve and sensory disturbances.
Guillain-Barré syndrome requires prompt medical attention, and early diagnosis is crucial for effective management. Despite its potential severity, many individuals with GBS experience a full recovery with appropriate medical care and rehabilitation. Regular monitoring and rehabilitation are essential for managing residual symptoms and optimizing long-term outcomes.
Collagen disorders

Collagen disorders
Collagen disorders refer to a group of conditions characterized by abnormalities in the production, structure, or function of collagen, a key protein that provides structural support to various tissues in the body, including skin, bones, tendons, and organs. These disorders can manifest in various ways, affecting different systems and organs. Understanding the symptoms, causes, and types of collagen disorders is crucial for accurate diagnosis and management.
Symptoms:
- Joint Pain: Collagen disorders may lead to joint pain, stiffness, and inflammation.
- Skin Changes: Abnormal collagen can affect the skin, resulting in changes such as hyperelasticity, thinning, or scarring.
- Gastrointestinal Issues: Some collagen disorders can involve the gastrointestinal tract, leading to symptoms like abdominal pain, diarrhea, or constipation.
- Vascular Problems: Abnormal collagen may affect blood vessels, leading to conditions such as aneurysms or vessel fragility.
- Eye Complications: In certain collagen disorders, the eyes can be affected, causing issues such as scleral thinning or changes in the cornea.
- Raynaud’s Phenomenon: Cold-induced color changes in the fingers or toes may occur due to vascular spasms.
- Organ Involvement: Collagen disorders can affect internal organs, leading to complications in the heart, lungs, kidneys, or other systems.
Causes:
- Genetic Mutations: Many collagen disorders are inherited, resulting from genetic mutations that affect the production or structure of collagen.
- Autoimmune Reactions: Some collagen disorders, such as rheumatoid arthritis or systemic lupus erythematosus, involve an autoimmune response where the immune system mistakenly attacks collagen and other tissues.
- Environmental Factors: Exposure to certain environmental factors, toxins, or infections may contribute to the development of collagen disorders.
Types:
- Ehlers-Danlos Syndromes (EDS): A group of genetic disorders characterized by hypermobility of joints, skin hyperelasticity, and tissue fragility. There are several subtypes of EDS with varying features.
- Marfan Syndrome: A genetic disorder affecting connective tissue, including collagen, leading to features like tall stature, long limbs, joint hypermobility, and cardiovascular abnormalities.
- Systemic Lupus Erythematosus (SLE): An autoimmune disease where the immune system can attack collagen and other tissues, causing inflammation and a range of symptoms affecting multiple organs.
- Rheumatoid Arthritis (RA): An autoimmune condition where the immune system attacks the synovium, a membrane that produces collagen in the joints, leading to joint inflammation and damage.
- Scleroderma: Characterized by excessive collagen production, leading to skin thickening, joint stiffness, and internal organ involvement.
- Polymyositis/Dermatomyositis: Inflammatory disorders affecting the muscles and sometimes the skin, involving the immune system’s attack on muscle tissue.
- Osteogenesis Imperfecta: A genetic disorder causing brittle bones due to abnormalities in collagen production.
Collagen disorders are often chronic and require ongoing management to alleviate symptoms and prevent complications. A multidisciplinary approach involving rheumatologists, geneticists, and other specialists is essential for comprehensive care. Early diagnosis and appropriate treatment strategies can significantly improve the quality of life for individuals with collagen disorders.
Multiple sclerosis
Multiple sclerosis
Multiple Sclerosis: Unraveling Symptoms, Causes, and Types
Multiple sclerosis (MS) is a chronic autoimmune disorder that affects the central nervous system (CNS), leading to a wide range of symptoms. It occurs when the immune system mistakenly attacks the protective covering of nerve fibers, disrupting communication between the brain and the rest of the body. Understanding the symptoms, causes, and types of multiple sclerosis is essential for diagnosis and management.
Symptoms:
- Fatigue: Persistent fatigue is a common symptom in individuals with multiple sclerosis. It can be overwhelming and may interfere with daily activities.
- Difficulty Walking: MS can affect the coordination and balance of an individual, leading to difficulty walking. This can manifest as stumbling, lack of coordination, or even muscle weakness.
- Numbness or Tingling: Many people with MS experience sensations of numbness, tingling, or a “pins and needles” feeling. These sensations can occur in various parts of the body.
- Muscle Weakness: Weakness in the muscles, often accompanied by tremors or spasms, is a common symptom. This can impact fine motor skills and overall strength.
- Vision Problems: MS can affect the optic nerve, leading to vision problems. This may include blurred or double vision, pain during eye movement, or even partial or complete loss of vision.
- Dizziness and Vertigo: Some individuals with MS experience dizziness or vertigo, a sensation of spinning or imbalance.
- Difficulty with Coordination and Balance: Coordination and balance issues are common, leading to challenges in activities requiring precise movements.
- Issues with Bowel and Bladder Control: MS can affect the nerves that control bowel and bladder function, leading to issues such as incontinence or difficulty emptying the bladder.
- Cognitive Changes: MS may impact cognitive function, causing problems with memory, concentration, and information processing.
- Emotional Changes: Mood swings, depression, and anxiety are common emotional changes associated with MS. Dealing with the challenges of the condition can also contribute to emotional distress.
Causes:
- Autoimmune Response: The exact cause of multiple sclerosis is not fully understood, but it is believed to involve an autoimmune response. The immune system mistakenly targets the myelin sheath, a protective covering around nerve fibers in the CNS, leading to inflammation and damage.
- Genetic Factors: There is a genetic component to MS, as individuals with a family history of the condition have a slightly higher risk. However, genetics alone do not determine the development of MS.
- Environmental Factors: Certain environmental factors, such as vitamin D deficiency, smoking, and viral infections, may contribute to the risk of developing MS. Exposure to these factors, especially during early life, may play a role in triggering the autoimmune response.
- Viral Infections: Some viral infections, including the Epstein-Barr virus, have been associated with an increased risk of developing multiple sclerosis. However, having a viral infection does not guarantee the development of the condition.
- Geographical Distribution: MS is more prevalent in certain geographical regions, suggesting a potential role of environmental factors. It is more common in higher latitudes, and the risk decreases closer to the equator.
Types:
- Relapsing-Remitting MS (RRMS):
– Characteristics: RRMS is the most common form, characterized by periods of relapse or exacerbation followed by periods of partial or complete recovery (remission).
– Symptoms: During relapses, new symptoms may appear or existing ones may worsen, while remissions involve a reduction or disappearance of symptoms.
- Primary Progressive MS (PPMS):
– Characteristics: PPMS is characterized by a gradual progression of symptoms without distinct relapses or remissions.
– Symptoms: Individuals with PPMS may experience a steady increase in disability over time.
- Secondary Progressive MS (SPMS):
– Transition: SPMS often develops from RRMS. After an initial phase of relapses and remissions, the disease transitions to a more progressive form.
– Symptoms: Symptoms gradually worsen, and disability accumulates over time.
- Progressive-Relapsing MS (PRMS):
– Characteristics: PRMS is a less common form with a steady progression of symptoms and occasional relapses.
– Symptoms: Disability accumulates steadily, and relapses may occur without full recovery.
- Clinically Isolated Syndrome (CIS):
– Characteristics: CIS is a single episode of neurological symptoms that lasts at least 24 hours.
– Risk of MS: Individuals with CIS may or may not develop MS. Further evaluation and monitoring are needed to determine the risk.
Early diagnosis and a multidisciplinary approach to management are crucial for improving the quality of life for individuals with multiple sclerosis. Regular monitoring, timely adjustments to treatment plans, and ongoing support can contribute to better outcomes and enhanced well-being. Additionally, lifestyle modifications, including a healthy diet, regular exercise, and stress management, may complement medical interventions in managing Multiple sclerosis.
Myopathies

Myopathies
Myopathies: Understanding Symptoms, Causes, and Types
Myopathies refer to a group of disorders characterized by muscle weakness and dysfunction. These conditions can affect various muscle groups and may result from genetic factors, autoimmune responses, metabolic abnormalities, or other underlying causes. Exploring the symptoms, causes, and types of myopathies is essential for accurate diagnosis and appropriate management.
Symptoms:
- Muscle Weakness: The hallmark symptom of myopathies is muscle weakness, which can affect different muscle groups. This weakness may be progressive and impact daily activities.
- Fatigue: Individuals with myopathies often experience fatigue, especially during or after physical activity. This fatigue is disproportionate to the level of exertion.
- Muscle Pain: Some myopathies may be associated with muscle pain, discomfort, or tenderness. This can vary in intensity and location.
- Difficulty Rising from a Sitting Position: Weakness in the proximal muscles, those closest to the trunk, can make it challenging to stand up from a seated position.
- Difficulty Climbing Stairs: Weakness in the leg muscles may result in difficulties climbing stairs or rising from a squatting position.
- Impaired Fine Motor Skills: Myopathies affecting the muscles of the hands and fingers can lead to difficulties with tasks requiring fine motor skills, such as buttoning shirts or writing.
- Muscle Stiffness: Stiffness or tightness in the muscles, especially after periods of inactivity, is a common symptom in certain myopathies.
- Contractures: Some myopathies may lead to the development of joint contractures, where muscles and tendons become shortened, limiting joint movement.
- Respiratory Complications (In Severe Cases): Progressive muscle weakness, particularly in the muscles involved in breathing, may lead to respiratory difficulties in advanced stages.
Causes:
- Genetic Factors: Many myopathies have a genetic basis, with mutations in specific genes affecting muscle structure or function. These genetic abnormalities may be inherited or occur spontaneously.
- Metabolic Abnormalities: Disorders affecting metabolism, such as glycogen storage diseases or mitochondrial myopathies, can lead to myopathy.
- Autoimmune Responses: Inflammatory myopathies, a subgroup of myopathies, result from an autoimmune response where the body’s immune system mistakenly attacks its own muscle tissues.
- Toxic Substances: Exposure to certain toxins, medications, or substances can cause myopathies. For example, the long-term use of certain cholesterol-lowering drugs known as statins may lead to muscle-related side effects.
- Endocrine Disorders: Hormonal imbalances, particularly related to the thyroid gland, can contribute to myopathy.
- Infections: In some cases, viral or bacterial infections may trigger or exacerbate myopathies.
- Nutritional Deficiencies: Inadequate levels of essential nutrients, such as vitamin D or certain minerals, can contribute to muscle weakness and myopathy.
- Inflammatory Processes: Inflammation within muscle tissues, either as part of an autoimmune response or due to other inflammatory conditions, can lead to myopathies.
Types:
- Muscular Dystrophies:
– Characteristics: Muscular dystrophies are a group of genetic disorders characterized by progressive muscle degeneration and weakness.
– Examples: Duchenne muscular dystrophy, Becker muscular dystrophy, limb-girdle muscular dystrophy.
- Inflammatory Myopathies:
– Characteristics: These myopathies result from inflammation within the muscles, often involving the immune system.
– Examples: Dermatomyositis, polymyositis, inclusion body myositis.
- Mitochondrial Myopathies:
– Characteristics: Mitochondrial myopathies involve dysfunction in the mitochondria, the cellular structures responsible for energy production.
– Symptoms: Muscle weakness, fatigue, and exercise intolerance are common features.
– Examples: Mitochondrial myopathy, Kearns-Sayre syndrome, Leigh syndrome.
- Metabolic Myopathies:
– Characteristics: These myopathies result from abnormalities in metabolic processes affecting energy utilization in muscle cells.
– Examples: Glycogen storage diseases, lipid storage myopathies.
- Endocrine Myopathies:
– Characteristics: Myopathies associated with hormonal imbalances, particularly those related to the thyroid gland.
– Examples: Hypothyroid myopathy.
- Toxic Myopathies:
– Characteristics: Myopathies caused by exposure to toxic substances, medications, or drugs.
– Examples: Statin-induced myopathy, alcohol-related myopathy.
- Congenital Myopathies:
– Characteristics: These myopathies are present from birth and result from genetic abnormalities affecting muscle structure or function.
– Examples: Nemaline myopathy, central core disease.
- Infectious Myopathies:
– Characteristics: Myopathies triggered or exacerbated by viral or bacterial infections.
– Examples: Coxsackievirus myopathy, HIV-related myopathy.
- Nutritional Myopathies:
– Characteristics: Myopathies resulting from nutritional deficiencies, such as deficiencies in vitamin D or certain minerals.
– Examples: Vitamin D deficiency myopathy.
Raynaud's disease
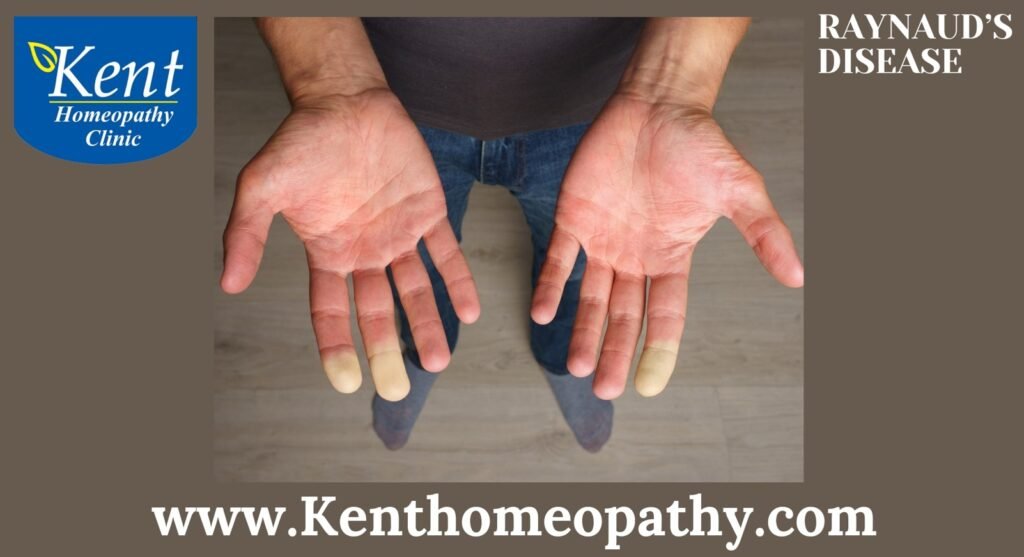
Raynaud's disease
Raynaud’s Disease: Unveiling Symptoms, Causes, and Types
Raynaud’s disease, also known as Raynaud’s phenomenon or Raynaud’s syndrome, is a vascular disorder that affects blood flow to certain parts of the body—usually the fingers and toes—resulting in episodes of reduced blood flow and color changes. Understanding the symptoms, causes, and types of Raynaud’s disease is essential for effective management and improved quality of life for those affected.
Symptoms:
- Color Changes in Extremities:
– The primary symptom of Raynaud’s disease is a sequence of color changes in the affected extremities. During an episode, the affected areas may turn white or pale, then blue or purple, and finally, as blood flow returns, they may become red.
- Cold and Numb Sensations:
– Individuals with Raynaud’s disease often experience sensations of cold and numbness in the affected areas during an episode.
- Throbbing or Tingling Sensations:
– After the episode resolves and blood flow returns, individuals may experience throbbing or tingling sensations in the affected extremities.
- Skin Ulcers or Sores:
– In severe cases, repeated episodes of reduced blood flow can lead to the development of skin ulcers or sores, particularly on the fingertips.
- Stress-Induced Episodes:
– Stress and emotional triggers can provoke or exacerbate Raynaud’s episodes.
- Limited Joint Mobility:
– Prolonged or severe cases of Raynaud’s disease may lead to limited joint mobility and deformities in the affected areas.
Causes:
- Vasoconstriction:
– Raynaud’s disease is primarily characterized by vasoconstriction, where the blood vessels narrow, limiting blood flow to affected areas.
- Primary vs. Secondary Raynaud’s:
– Primary Raynaud’s disease, the more common form, occurs without an underlying medical condition. Secondary Raynaud’s is associated with other conditions, such as scleroderma, lupus, or rheumatoid arthritis.
- Blood Vessel Abnormalities:
– Abnormalities in the smaller arteries that supply blood to the skin contribute to the vasoconstriction seen in Raynaud’s disease.
- Nerve Abnormalities:
– Dysfunction of the nerves controlling blood vessel activity may play a role in the development of Raynaud’s.
- Hypersensitivity to Cold or Stress:
– Individuals with Raynaud’s may have an exaggerated response to cold temperatures or emotional stress, triggering episodes.
- Genetic Factors:
– There may be a genetic predisposition to Raynaud’s disease, as it often runs in families.
Types:
- Primary Raynaud’s Disease:
– Also known as Raynaud’s phenomenon, this is the more common and less severe form. It occurs without an underlying medical condition and is often less likely to lead to complications.
- Secondary Raynaud’s Disease:
– Also called Raynaud’s syndrome, this form is associated with other medical conditions, most commonly autoimmune disorders like scleroderma, lupus, or rheumatoid arthritis. Secondary Raynaud’s tends to be more severe and may involve complications.
- Limited Cutaneous Systemic Sclerosis (SSc):
– Raynaud’s disease associated with limited cutaneous systemic sclerosis (SSc) is a subtype linked to the autoimmune disorder scleroderma. It may involve skin thickening and tightness, particularly in the fingers.
- Diffuse Cutaneous Systemic Sclerosis (SSc):
– In this subtype associated with scleroderma, skin changes are more widespread, affecting not only the fingers but also the arms, face, and trunk.
- Overlap Syndrome:
– Some individuals may experience an overlap syndrome, where features of Raynaud’s disease are present along with symptoms of other autoimmune conditions.
Contact to know more
Contact
Timings
Monday to Saturday:
11:00 AM to 02:30 PM
06:30 PM to 09:00 PM
